Ovarian epithelial cancer begins in the tissue that covers the ovaries — the reproductive glands that produce eggs. Although women can be diagnosed with different types of ovarian cancer, such as germ cell and stromal tumors, ovarian epithelial cancer is the most common, accounting for about 90% of ovarian cancer patients. This cancer typically occurs in post-menopausal women (approximately age 50 and up), with about half of the women diagnosed at age 63 or older. More Caucasian women are affected than other races.
In most cases, ovarian cancer isn’t diagnosed until it has reached an advanced stage. This is because early-stage symptoms often mimic symptoms of common stomach and digestive illnesses. Or, the patient isn’t experiencing symptoms at all. Knowing what to look for and catching it early is best since this is when treatment can bring a more favorable outcome.
Learn more below about what to look for and what types of treatments are available for ovarian cancer.

Learn about the various types of procedures that may be used to diagnose ovarian cancer. Initial tests may be run by your gynecologist or another medical professional.

To plan the best treatment for ovarian cancer your gynecologic oncologist needs to know the extent (stage) of the disease.
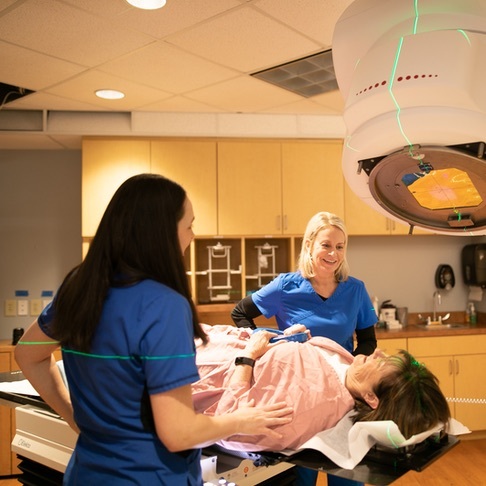
Treatment options depend on several factors, including the type, stage, and grade of the cancer. Learn more about ovarian cancer treatments.
A cancer risk factor is anything that increases your chance of developing a disease like ovarian cancer. It’s important to understand, however, that having a risk factor does not mean that you will get cancer; not having risk factors doesn't mean that you will not get cancer. With that said, it is important to be aware of the factors that could increase your risk of ovarian cancer and what you can do to help lower your risks.
There are a variety of factors that can increase your risk of ovarian cancer. Most of these risk factors can’t be controlled; however, those factors that involve personal lifestyle choices can be changed.
Common risk factors for ovarian cancer can include:
Family history. Ovarian cancer in a first-degree relative (mother, daughter, or sister) can put you at an increased risk for ovarian cancer. A family history of certain other types of cancer, including breast cancer, can be linked to an increased risk of ovarian cancer.
Genetics. Inherited changes in the BRCA1 or BRCA2 genes, or one associated with Lynch syndrome, can raise the risk of developing ovarian cancer. Hereditary ovarian cancer makes up about 20% of all cases of ovarian cancer.
Age. The risk of developing ovarian cancer increases with age. Most ovarian cancers develop after menopause.
Weight. Studies show that obese women have a higher risk of developing ovarian cancer.
Endometriosis. This condition may increase the risk of certain types of ovarian cancer, including clear cell and endometrioid ovarian cancers.
Hormone replacement therapy. Some studies suggest that women who use estrogen replacement after menopause are at an increased risk for ovarian cancer.
Reproductive history and infertility. Beginning menstruation at an early age or starting menopause at a later age, or both, may increase the risk of ovarian cancer. Women who had full-term pregnancies, before the age of 26, are at a lower risk than women who had their first full-term pregnancy after age 35. Women who have never carried a pregnancy to term are also at a higher risk.
While there is no guarantee that any woman won’t get ovarian cancer, there are steps that can be taken to help reduce any risk factors that can be avoided.
Here are some things you can do to lower your risk for ovarian cancer and other types of cancer:
Changing lifestyle or eating habits to choose healthier choices
Avoiding things known to cause cancer, like smoking and talcum powder
Getting pregnant and breastfeeding after giving birth
Taking oral contraceptives
Undergoing genetic testing if any of your first-degree relatives (grandmother, mother, daughter; sister) have been diagnosed with ovarian or breast cancer. If the test shows you are BRCA positive, you might discuss removing your ovaries after your childbearing years are complete to reduce the likelihood of cancer developing.
Keep in mind that genetic testing and preventive gynecological surgery (called prophylactic BSO) is only recommended for patients who have a strong family history of ovarian or breast cancer. The decision to undergo either comes down to a personal choice only you can make.

Unfortunately, the later ovarian cancer is found, the more difficult it is to treat. This is why it’s good for patients to be as educated as possible regarding detecting ovarian cancer early when it is more likely to be treated successfully.
Signs and symptoms for ovarian cancer may include:
Gastrointestinal changes, such as gas, bloating, or constipation
Changes in bowel movements, ruling out a virus or other gastrointestinal condition
Trouble eating or feeling full
Pain or discomfort (such as pressure) in the abdomen or pelvis
The need to urinate more urgently or frequently, ruling out a urinary tract infection first
Pelvic or back pain
Changes in menstruation
Bleeding vaginally after menopause
Pain during sexual intercourse
Fatigue
Nausea or vomiting
Swelling, pressure, or pain in the abdomen
Again, these symptoms can certainly be caused by conditions other than ovarian cancer. With that said, it is important that they aren’t ignored. If you notice persistent symptoms, especially ones that last for more than a few weeks, we urge you to visit your gynecologist for a pelvic exam so a proper diagnosis can be made and treatment can be started, if necessary.
Quickly and efficiently build the materials you need to support your inbound marketing strategy. Drag and drop building blocks including testimonials, forms, calls-to-action, and more.