There are various treatment options available for lung cancer, based on the size, type, and stage of your lung cancer. Recently a new study has been added to the lung cancer diagnosis process that determines if there are any genetic mutations present, called biomarkers.
Based on each patient’s specific case, the treatments for lung cancer will vary but may include: targeted therapy, immunotherapy, surgery, chemotherapy, and radiation therapy. A combination of these treatment types may be used in your care plan. Clinical research trials for lung cancer may also be available based on your biomarker status.
Surgery is commonly used to treat early stages of non-small cell lung cancer (NSCLC). Although it may sometimes be used for some early-stage small cell lung cancer (SCLC), it is rarely used as the primary treatment. That’s because most patients don’t find out they have SCLC until it has metastasized (spread) past the lungs at the time of diagnosis. Lung cancer surgery can involve removing a portion of the lung or the entire lung through procedures such as lobectomy, segmentectomy, wedge resection, and pneumonectomy. It can also include cryotherapy, or freezing of the cancerous cells to kill them.
Even if the lung surgeon removes all the cancer that can be seen at the time of the operation, you may be given other treatments after surgery to kill any cancer cells that may remain.
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Since lung cancer tends to spread quickly throughout the body, chemo is often given as it reaches cancer cells that have extended past the lungs. The way the chemotherapy is given depends upon the type and stage of the cancer being treated.
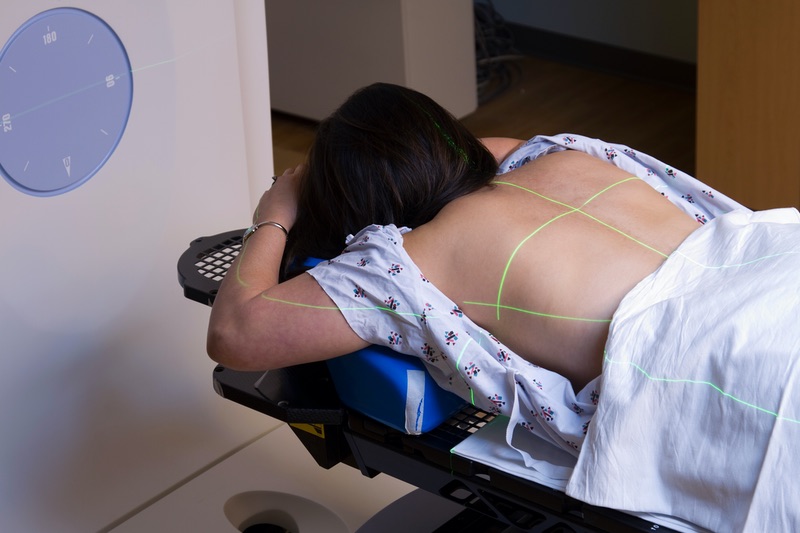
Radiation therapy is a treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or prevent them from growing. External beam radiation therapy is commonly used during the course of a patient’s lung cancer treatment. If you or someone you love has been diagnosed with lung cancer – small cell or non-small cell – you have options for where to receive radiation therapy. Find a location that’s close to you in the Atlanta area.
External radiation therapy uses high-intensity beams of radiation, directed at a very specific area of the body, to kill cancer cells and shrink tumors. Because lung cancer can be present in a large area, it’s not used for every patient.
Patients who meet one of the following criteria are often good candidates for external beam radiation therapy for non-small cell lung cancer:
A tumor that can’t be removed because of its size or location.
If a patient’s health doesn’t allow them to undergo surgery.
Before surgery to try to shrink the tumor which makes it easier to remove.
After surgery to kill any small areas of lung cancer that might not have been taken out.
Patients with small cell lung cancer have radiation therapy used in a different way than non-small cell lung cancer patients. These patients receive radiation for one of these conditions:
To treat the tumor and lymph nodes in the chest. If chemotherapy has begun and radiation is given over that same period of time, this is called concurrent chemoradiation. This, however, can’t be tolerated by all patients.
For those who have extensive disease, or for those with limited stage lung cancer who couldn’t tolerate chemoradiation, radiation therapy can be given after the chemotherapy phase of treatment is complete.
To help lower the chances of cancer spreading to the brain, prophylactic (preventative) cranial irradiation may be given.
What’s best for each patient will be decided during the treatment planning phase. There are several types of external beam radiation that could be used to treat lung cancer, depending on where the cancer is located.
Stereotactic Body Radiotherapy (SBRT)
Stereotactic Body Radiotherapy (SBRT) is an advanced type of radiation technology most often used to treat early-stage lung cancers when surgery isn’t an option. Rather than administering a small dose of radiation each day for several weeks, SBRT uses very focused beams of high-dose radiation, which are given in fewer treatments. Several beams are aimed at the tumor from different angles. A specially-designed body frame is used to help reduce movement of the lung tumor during breathing so it can be precisely targeted.
Intensity-Modulated Radiation Therapy (IMRT)
This type of external beam radiation called Intensity Modulated Radiation Therapy (IMRT) allows precise targeting of tumor cells. IMRT also makes it possible for the radiation oncologist to vary the intensity of some of the beams of radiation to focus more carefully in some areas than in others. This type of radiation may also be used to treat lymph nodes in the chest where lung cancer is likely to spread.
Stereotactic Radiosurgery (SRS)
Stereotactic radiosurgery is a type of external radiation therapy used to treat lung cancer that has limited spread to the brain.
For SRS, a custom head frame is made to keep the head very still during the radiation treatment. A machine delivers a single large dose of radiation directly at the tumor(s) in the brain.
Fractionated SRS may be used to deliver large doses of radiation over three to five treatment sessions for multiple lesions or those near critical areas of the brain.
3-Dimensional Conformal Radiation Therapy
Three-dimensional conformal radiation therapy (3D-CRT) allows doctors to direct radiation beams to conform to the shape of the tumor. 3D conformal radiation uses images from CT, MRI, and PET scans to precisely plan the treatment areas through a process called simulation. A computer program is then used to analyze the images and to design radiation beams that conform to the shape of the tumor. The precise shaping makes it possible to use higher doses of radiation to the tumor while sparing normal tissue.
Possible Side Effects of External Lung Cancer Radiation
Before undergoing radiation therapy, talk with your radiation oncologist about what to expect, including the possible short-term and long-term side effects. Side effects will depend on factors such as the treatment area, total dose of radiation, type of radiation therapy used, and whether chemotherapy is given at the same time (chemoradiation).
Common side effects of radiation therapy for lung cancer can include:
Feeling tired
Hair loss specific to the area receiving the radiation
Red, dry, or peeling skin at the radiation site
Trouble swallowing
Cough
Nausea and vomiting
Shortness of breath
Loss of appetite and weight loss
Although most side effects go away on their own, some may last a long time or become permanent. Talk to your oncologist or radiation therapist right away if you notice any side effects so steps can be taken to reduce or relieve them.
Immunotherapy drugs are used to help the body’s immune system kill cancer cells. Currently, the lung cancer immunotherapy used to treat patients with NSCLC and some patients with advanced SCLC belong to a class called checkpoint inhibitors. Immune checkpoints are molecules on the immune cells that can start or stop an immune response. Your body’s immune system uses these molecules to help determine what cells are foreign (not normal). Cancer cells have found ways around this system by hiding from your body’s natural immune system or by weakening the immune system itself. Immunotherapy drugs allow the immune system to recognize and destroy the cancer cells. Immunotherapy is normally given intravenously (through an IV) every 2 to 3 weeks.
Targeted therapy is a type of treatment that uses drugs or other substances to identify and attack specific cells based on their genetic makeup. The biomarker testing that is conducted during the diagnosis and staging process identifies any targeted therapies for NSCLC that may be available. The type of genetic mutation that’s found will direct the first line of treatment that’s recommended. If no biomarkers are found, a different approach will be recommended.
Because of this precision, healthy cells are left alone, reducing the side effects that often come with other types of treatment, such as chemotherapy and radiation therapy. Monoclonal antibodies, tyrosine kinase inhibitors, and mammalian target of rapamycin (mTOR) inhibitors are three types of targeted therapy being used to treat certain types of lung cancer.
An endoscope is a thin, tube-like instrument used to look at tissues inside the body. An endoscope has a light and a lens for viewing and may be used to place a stent in a body structure to keep the structure open. Endoscopic stent placement can be used to open an airway blocked by abnormal tissue. In some cases, follow-up tests may be needed.
Laser therapy is a cancer treatment that uses a laser beam (a narrow beam of intense light) to kill the cancer cells. This treatment is sometimes used to open up the airways of patients whose cancer makes it hard to breathe.
While you are under general anesthesia, the oncologist inserts the laser with a bronchoscope and then aims the beam at the tumor to burn it away. Treatment may be repeated as needed.
There are times when certain tests that were done to diagnose the cancer, or to find out the stage of the cancer, may be repeated. In some cases, it’s to evaluate whether treatment appears to be successful. In others, the results are used to help make decisions about whether to continue, change, or stop treatment. This process is sometimes called re-staging.
Even after treatment has ended, some of the tests will continue to be done from time to time. The results of these tests, sometimes called follow-up tests or check-ups, can show if your condition has changed or if the cancer has returned.

Quickly and efficiently build the materials you need to support your inbound marketing strategy. Drag and drop building blocks including testimonials, forms, calls-to-action, and more.