ProstRcision is a specific prostate cancer treatment, developed by one of our own radiation oncologists, that uses a combination of two types of radiation therapy for a high rate of success. The documented 10-year and 15-year high success rates, combined with no cutting of the prostate, and very few side effects are why over 16,000 men from all 50 states, and over 40 countries have chosen ProstRcision.
Here are the reasons that patients and providers choose ProstRcision:
Two kinds of radiation – Utilizing both seed implants and conformal beam irradiation means ProstRcision attacks prostate cancer from every angle.
Standards and procedures – Strict adherence to procedures ensure that the most efficient process is carried out every time.
A world-class information database – We have tracked progress on every patient we have ever treated and can leverage this information to tailor a man’s treatment.
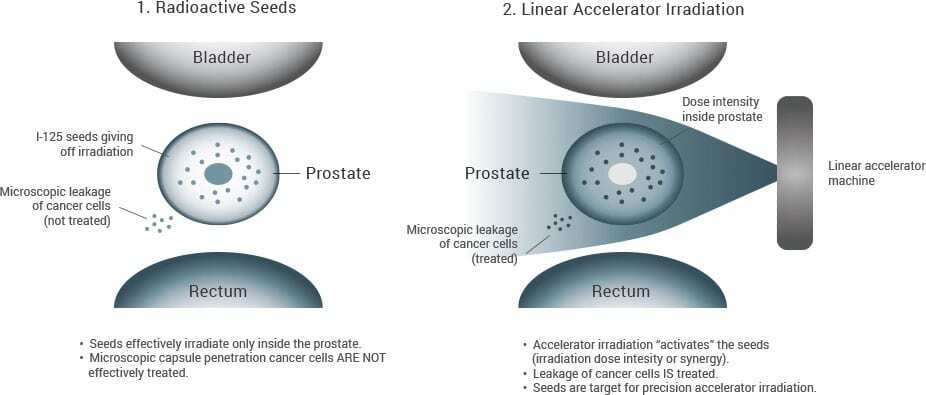
The ProstRcision procedure begins when a physician implants tiny radioactive seeds into the prostate. Since the seeds are only 1/5 of an inch in length and as thin as a pencil lead, physicians can position them directly in the tumor and away from important muscles and nerves. These seeds emit most of their radiation over the course of a few months but will continue to release radiation for up to one year. When we say ProstRcision can attack the cancer with pinpoint accuracy, it’s because the area surrounding the seeds is hit with a tremendous amount of radiation, but a few millimeters away, the radiation level drops off rapidly.
Since the prostate does not show up on an X-ray, the precisely placed radioactive seeds not only release radiation to kill the cancer, but they serve to map out the prostate so it can be seen on X-ray as well. In addition to these small silver seeds, physicians inject several slightly larger and thicker gold seeds into the prostate. These gold seeds also help to outline the prostate on X-rays, so the doctor can plan the second step of the ProstRcision process – the delivery of targeted irradiation.
Seed implants are an excellent way to destroy cancer within the prostate, but they do have limitations. They don’t effectively kill any cancer that may have leaked outside the prostate (called microscopic capsule penetration). Further, because of the amount of close-range radiation these seeds give off, they cannot be placed right next to the urethra without damaging it. Importantly, studies show that over 41% of men with prostate cancer have cancer on or near the urethra. This is why we follow the seed implant with another type of radiation called linear accelerator irradiation. The additional radiation delivered by an accelerator ensures that all the cells are killed within the prostate, because leaving even one cell, healthy or cancerous, could allow the cancer to come back over time.
One or two methods are used to deliver linear accelerator irradiation – either conformal beam (where the beam of radiation is shaped into an exact outline of each patient’s prostate) or the Intensity Modulated Radiotherapy Technique (IMRT). IMRT allows for better control over the dose of radiation and can potentially keep the nearby organs from being over-exposed while focusing the radiation on the prostate.
 When it comes to treating your prostate cancer, there are a handful of different routes to take. When making the decision between surgery, radiation therapy, hormone therapy, and all other options, you must consider both the short-term and long-term positives and negatives of each approach.
When it comes to treating your prostate cancer, there are a handful of different routes to take. When making the decision between surgery, radiation therapy, hormone therapy, and all other options, you must consider both the short-term and long-term positives and negatives of each approach.
You should also get a better understanding of your particular case of cancer; some forms of prostate cancer can be slow-growing and never bother you during your natural lifespan, while others can be extremely aggressive within a few years. Read on to learn more about ProstRcision, a treatment method for prostate cancer, and who might be a prime candidate for this form of treatment—16,000+ other men were!
At RCOG, how we treat prostate cancer and the chance of curing your prostate cancer hinges on your particular cancer findings, especially your prostate pathology report.
You are a prime candidate for ProstRcision if you:
Prefer an alternative to surgery that offers a comparably high cure rate
Place a high priority on curing your cancer
Are looking for a treatment supported with outcome data as opposed to verbal assurances
Are interested in options that provide compelling published outcome data
Prioritize cure over convenience
Want to minimize effects of sexual function and not experience urinary issues
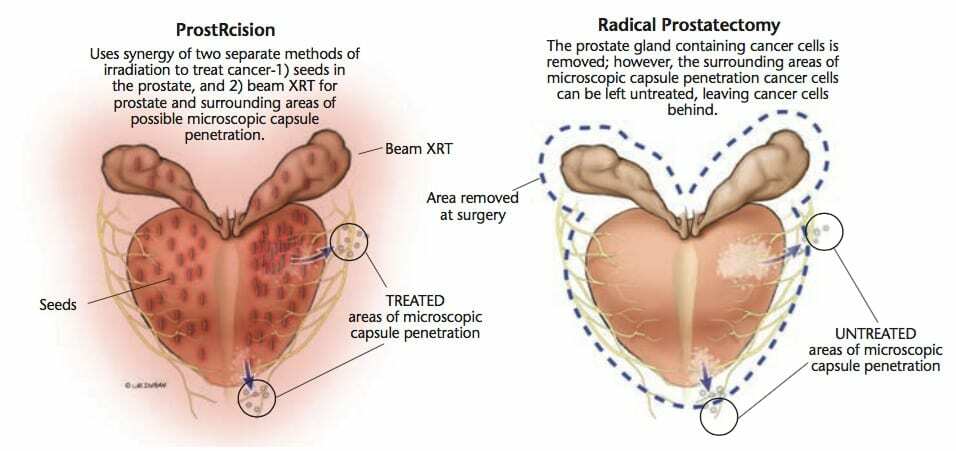
How do you choose between ProstRcision and a radical prostatectomy? Just like you would compare any two treatments: which one gives you the best chance of zero PSA 10 years later for your particular case of prostate cancer. There is no one cure rate for surgery because it varies with the skill of the urologist. Also, microscopic capsule penetration is probably a bigger problem for surgery than ProstRcision. You should also look at the other two big issues: urinary incontinence and loss of sexual function.
ProstRcision is an outpatient procedure meaning that it does not require a hospital stay. Even with the delicate nature of implanting radioactive seeds into the prostate, the procedure itself doesn’t take very long – usually about 45 minutes. Most patients go home within hours. While this is the typical outcome, every patient is unique, and it is imperative to consult with your ProstRcision physician on your treatment.
Performed by a urologist and a radiation oncologist, the seed implant is an outpatient procedure that lasts approximately 45 minutes. Patients are given general anesthesia, and the man’s legs are placed in stirrups. Then an ultrasound probe, which is connected to a television monitor, is inserted into the rectum. To get the seeds in place, and while watching the monitor, long hollow needles are inserted through the perineum (the area between the testicles and the rectum) and into the prostate.
Next, a seed implant device is attached to a needle, and seeds are injected into the prostate. The process is repeated until all of the seeds have been injected. The number of seeds needed depends on the size and shape of the prostate, as well as the severity of the cancer.
The average number is 74 seeds, but we have implanted as few as 45 and as many as 230.
After all the seeds have been injected, the urologist performs a cystoscopic exam, which is the insertion of a tube through the urethra and into the prostate and bladder to check on these organs. Once the urologist sees that everything is okay, a urinary catheter is inserted, and the patient is sent to the recovery room, where he is awakened.
The patient returns to RCOG the following day to have the urinary catheter removed.
Since cancer cell leakage cannot be detected prior to completing any treatment, we use follow-up linear accelerator irradiation to make sure we target the entire area, guided by the implanted seeds. This follow-up treatment begins 21 days after the seed implant and is delivered slowly over a six to seven-week period. Treatment is similar to getting a pelvic X-ray each day and lasts approximately 10 minutes. Patients can resume normal daily activities immediately after each treatment.
When compared to other treatments available today for prostate cancer, ProstRcision patients experience minor, if any, side effects. One of the great advantages of ProstRcision is that important muscles and sex nerves are not cut, so men stand an excellent chance of maintaining bladder control and sexual function. Additionally, since ProstRcision is a relatively fast outpatient procedure, patients enjoy a high quality of life, and can go back to work or other regular activities, usually the day after implant. Other than Tylenol, most patients don’t usually need medication during the recovery time.
However, there are a few minor side effects that some patients experience following ProstRcision treatment. The most commonly reported side effects are a weak urine stream and more frequent urination, and more urgency. It’s important to note that these symptoms vary from patient to patient and are usually connected to the size of the patient’s prostate and the severity of his urination symptoms before treatment.
Patients who experience these symptoms usually see them decrease over the next 6-12 months as the prostate shrinks. Some patients also report a feeling of fatigue that may last for several months after treatment. It is unusual for patients to experience side effects more than 24 months after ProstRcision.
We see patients from around the United States who would like to receive the unique ProstRcision therapy. If you or a loved one would like to discuss your specific diagnosis, you can speak to a care team member who can arrange a consultation.

Make an informed prostate cancer treatment decision. Our 40-page, comprehensive guidebook provides answers to our most frequently asked questions from men diagnosed with prostate cancer, and compares various treatment methods, cure rates and side effects. Our team can also connect you with one of our oncologists at no cost.
Quickly and efficiently build the materials you need to support your inbound marketing strategy. Drag and drop building blocks including testimonials, forms, calls-to-action, and more.